Hip arthroscopy is one of the most advanced and minimally invasive surgical techniques in modern orthopedics. Because it requires smaller incisions, results in minimal scarring, and is typically associated with less post-operative pain than traditional open surgery, it has become a widely accepted approach for treating a variety of hip conditions.
At Detroit Ortho Doc, our hip specialists prioritize joint preservation and non-surgical care whenever possible. When conservative treatments are no longer effective, we utilize advanced hip arthroscopy techniques as a precise, minimally invasive solution to restore function, relieve pain, and protect the natural hip joint.
Hip pain can be frustrating, limiting, and often misunderstood, especially when it stems from damage deep within the joint. Conditions like acetabular labrum tear, anterior labral tear, or anterosuperior labral tear can cause persistent discomfort, instability, and reduced performance. Therefore, hip arthroscopy is a joint-preserving solution designed to restore function and relieve pain.
This comprehensive guide explains everything you need to know about hip arthroscopy surgery, including indications, recovery, benefits, risks, and how it compares to joint replacement, helping you make an informed decision about your care.
After reading this, consult our orthopedic specialists at DetroitOrthoDoc to get a personalized plan for your Hip Arthroscopy.
What Is Hip Arthroscopy?
Hip arthroscopy is a minimally invasive surgical procedure used to diagnose and treat conditions within the hip joint. Through small incisions, surgeons insert a tiny camera called an arthroscope along with specialized instruments to repair damaged cartilage, reshape abnormal bone, and address labral injuries, without the need for traditional open surgery.
This technique reflects how modern medical technology has transformed orthopedic care, making procedures more precise, recovery faster, and outcomes more predictable. The use of small incisions and real-time camera visualization, central to the concept of arthroscopy, represents a major advancement in contemporary orthopedic surgery, allowing effective treatment while minimizing tissue disruption.
It is commonly performed for labral damage such as acetabular labrum tear, anterior superior labral tear hip treatment, and cartilage abnormalities that cause pain, stiffness, or mechanical symptoms. Today, hip arthroscopy surgery accounts for a growing share of hip orthopedic procedures, with studies estimating that over 60–70% of hip preservation surgeries are now performed arthroscopically, reflecting its effectiveness and lower complication rates compared to open approaches.
Anatomy of the Hip Joint
The hip is a ball-and-socket joint designed for stability and motion. It consists of:
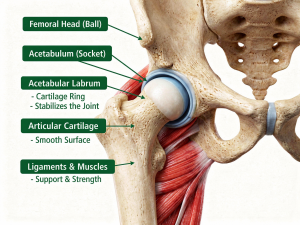
- Femoral head (ball)
- Acetabulum (socket)
- Acetabular labrum – a ring of cartilage that deepens the socket and stabilizes the joint
- Articular cartilage – smooth tissue allowing frictionless movement
- Ligaments and muscles that support mobility and strength
A tear in the labrum, such as an anterior labral tear or anterosuperior labral tear, disrupts joint stability and alters biomechanics, often leading to pain during rotation, sitting, or athletic activity. However, due to complex hip anatomy, each part can face a tear due to a sudden impact, injury or trauma. Injuries to different parts call for different treatment approaches which will be discussed in the later sections.
Different Types of Hip Tears and What They Mean?
| Term | What It Means | Clinical Significance |
| Acetabular Labrum Tear | Any damage to the labrum, including fraying, partial tears, or complete detachment from the socket. | Can cause hip pain, clicking, catching, and instability; often requires targeted evaluation to prevent joint deterioration. |
| Anterior Labral Tear | A tear located at the front (anterior) portion of the labrum, commonly associated with hip flexion and rotation movements. | Frequently presents as groin pain and discomfort during sitting, walking, or athletic activities. |
| Anterosuperior Labral Tear | A tear in the front-top (anterosuperior) region of the labrum, the most common site of labral injury. | Often linked to femoroacetabular impingement (FAI) and is a common indication for hip arthroscopy and labral repair. |
When Does the Hip Joint Need Surgery?
Not all hip labral conditions require surgery. The decision to proceed with surgical intervention depends on symptom severity, functional limitations, the extent of structural damage, and the patient’s response to non-surgical care. Physicians also assess factors such as pain frequency, intensity, mechanical symptoms (such as clicking or catching), and joint-related sounds before making a recommendation.
At our facility, extensive screening, including detailed physical examinations, X-rays, ultrasound scans, and other advanced diagnostic tests are performed to ensure that surgery is recommended only when all conservative treatment options haven’t been effective. However, many patients improve with conservative treatment focused on joint preservation. Below is how the surgical need varies across common labral conditions:
1. Acetabular Labrum Tear
Not all labral tears require surgery. Small or stable tears may respond well to physical therapy, activity modification, and inflammation control. Surgery is considered when pain persists, mechanical symptoms develop, or the tear compromises joint stability despite conservative care.
For Acetabular Labrum tear, surgery is needed, if non-surgical care fails. The preferred method is Hip Arthroscopy.
2. Anterior Labral Tear
Anterior labral tears often cause groin pain and discomfort with hip flexion or rotation. Many patients improve with structured rehabilitation and movement correction. Surgery may be recommended when the tear causes ongoing pain, clicking, or limits daily function after non-surgical treatment. The preferred surgical method for this type of tear is arthroscopic labral repair via hip arthroscopy.
3. Anterosuperior Labral Tear
This is the most common labral tear location and is frequently associated with femoroacetabular impingement (FAI). Because structural bone abnormalities often contribute to these tears, non-surgical care alone may not fully resolve symptoms. Hip arthroscopy is commonly recommended when imaging confirms impingement and symptoms persist. Surgery is often recommended when conservative care fails. For the majority of hip conditions hip arthroscopy is preferred. Before surgery, many patients also improve with:
- Activity modification
- Targeted physical therapy
- Anti-inflammatory care
- Injection therapy
However, when structural damage exists, such as a confirmed labral tear or cartilage defect, non-surgical care may relieve symptoms temporarily but cannot correct the underlying problem.
Our Approach Before Opting for Surgery (Detroit Ortho Doc Philosophy)
At Detroit Ortho Doc, we prioritize natural joint preservation and non-surgical solutions before recommending arthroscopy hip surgery. Surgery is considered only when conservative options have been exhausted and imaging confirms a correctable structural issue.
Non-Surgical Strategies We Use First
- Advanced Diagnostic Evaluation: High-resolution imaging and biomechanical assessment help identify whether pain is truly labral or coming from surrounding structures.
- Targeted Physical Therapy: Therapy focuses on hip stability, mobility balance, and muscle coordination to reduce joint stress and prevent worsening injury.
- Activity & Load Modification: Adjusting movement patterns can significantly reduce symptoms caused by labral overload or early cartilage damage.
- Injection-Based Therapies: Diagnostic or therapeutic injections help confirm pain sources and may delay or prevent the need for surgery.
When these approaches fail to restore function, hip arthroscopy for labral tear becomes a valuable next step.
Hip Arthroscopy vs Total Hip Replacement
In orthopedics, the choice of surgical method depends on several factors. For each individual the treatment option may vary because of:
a) their individual condition
b) the long-term goal
c) the damage posed to the joint.
In most cases, Hip Arthroscopy is a method preferred for younger patients with structural issues of labral tears of hip impingement. On the other hand, total hip replacement is a method when the entire hip joint has faced degeneration, or the patient is facing severe arthritis. Total hip replacement surgery also offers significantly long-term pain relief but with a longer rehab period. However, understanding hip arthroscopy vs total hip replacement is critical.
Hip Arthroscopy is ideal when:
- Joint cartilage is largely preserved
- Pain is mechanical or activity-related
- The goal is joint preservation
- Total hip replacement is preferred when:
- Advanced arthritis is present
- Cartilage loss is widespread
- Pain is constant and progressive
In many cases, hip arthroscopy vs hip replacement is not a competition, it’s about choosing the right solution for the right condition. Below is a table on how both procedures differ from each other along multiple aspects:
| Aspect | Hip Arthroscopy | Total Hip Replacement |
| Procedure Type | Minimally invasive, joint-preserving surgery | Open surgery replacing the entire hip joint |
| Primary Goal | Repair or preserve natural hip structures (labrum, cartilage, bone shape) | Replace damaged joint with artificial components |
| Incisions | Small keyhole incisions (typically 2–4) | Large surgical incision |
| Structures Treated | Labral tears, cartilage damage, impingement, loose bodies | Severe arthritis, advanced joint degeneration |
| Joint Preservation | Preserves the native hip joint | Native joint is removed |
| Best For | Younger, active patients with structural hip problems | Older patients with end-stage arthritis |
| Pain Relief Timeline | Gradual improvement over weeks to months | Often immediate relief after recovery |
| Hospital Stay | Often outpatient or same-day discharge | 1–3 days typical |
| Recovery Time | Faster recovery; return to activities in weeks to months | Longer recovery; full rehab may take months |
| Longevity of Outcome | Depends on joint health and correction of mechanics | Artificial joint lifespan 15–25 years |
| Revision Surgery Risk | Lower when joint preserved early | Possible revision needed over time |
| Impact on Sports/Activity | Allows return to many sports and high-level activities | High-impact activities often discouraged |
| Common Risks | Temporary nerve irritation, stiffness, persistent pain | Infection, dislocation, implant wear |
| Why It’s Chosen | Treats the cause while maintaining natural anatomy | Last-resort option for irreversible joint damage |
Signs Your Hip Pain Needs A Surgical Procedure
Many people live with hip pain longer than they should, often hoping it will resolve on its own. But when discomfort becomes constant, interferes with daily life, or no longer responds to treatment, it may be your body signaling a more serious underlying issue.
Hip replacement surgery isn’t just for older adults, it’s recommended whenever joint damage becomes severe enough to limit mobility, independence, and quality of life. Below are the most telling signs that it’s time to discuss hip replacement surgery with your orthopedic specialist.
1. Persistent, Severe Hip Pain That Never Fully Goes Away
One of the biggest red flags is pain that doesn’t improve with rest. If your hip aches even when you’re sitting, lying down, or trying to sleep, it may indicate advanced joint degeneration. This type of constant pain often suggests the cartilage is significantly worn down, leading to inflammation and bone irritation that can only be relieved through surgical intervention.
2. Difficulty Performing Normal Daily Activities
When simple movements, walking across the room, bending to tie your shoes, climbing stairs, or getting in and out of a car, start feeling like a challenge, your hip joint may be losing its functional capacity. You shouldn’t struggle through activities that used to be effortless. If daily mobility becomes painful or restricted, it’s a key indicator that the joint is failing and may require replacement.
3. Stiffness That Limits Your Range of Motion
Stiffness that makes it hard to rotate your leg, lift your knee, or move freely is often tied to advanced arthritis. If you experience tightness in the morning or after resting, or if your hip feels “stuck,” it signals that inflammation and joint damage are progressing. Over time, stiffness can become so restrictive that even basic movements feel mechanically blocked.
4. Grinding, Clicking, or Locking Sensation
A grinding or clicking feeling inside the hip may indicate bone-on-bone contact, one of the clearest signs that cartilage has worn away. Locking or catching sensations also point toward structural damage that will not heal without surgical repair. These mechanical symptoms typically worsen over time and are strong indicators for hip replacement.
5. Pain Radiating to the Groin, Knee, or Buttocks
Hip problems don’t always cause pain exactly where you expect. Many patients feel discomfort spreading to the groin, outer thigh, buttocks, or even down toward the knee. This “referred pain” happens because the hip joint shares nerve pathways with surrounding regions. Persistent radiating pain often signals significant joint damage.
6. Increasing Dependence on Assistive Walking Devices
If you’re relying more on a cane, walker, or holding onto furniture for support, it suggests your hip can no longer bear weight effectively. This gradual dependency reflects worsening instability and joint deterioration. When mobility aids become essential instead of occasional, it’s time to consult a specialist about surgical options.
7. Limping or an Altered Gait
Chronic hip degeneration forces your body to compensate, often resulting in an uneven stride or noticeable limp. This altered gait can place extra stress on your spine, knees, and opposite hip, creating additional problems. A worsening limp is a functional sign that the damaged joint is affecting your overall biomechanics.
8. Conservative Treatments No Longer Provide Relief
Before recommending surgery, doctors typically suggest non-surgical treatments like NSAIDs, steroid injections, physical therapy, activity modification, or rest. If these measures stop working, or only offer very temporary relief, the joint damage is likely too advanced for conservative care. This plateau is a common turning point when hip replacement becomes the most effective option.
9. Imaging Shows Bone-on-Bone Contact
X-rays, MRIs, or CT scans that reveal significant joint space loss or bone touching bone provide conclusive evidence of severe arthritis or degeneration. When imaging shows advanced structural damage, continued conservative treatment is unlikely to help. Bone-on-bone contact is one of the most definitive medical indicators for hip replacement.
10. Declining Quality of Life
Ultimately, the biggest sign that you may need hip replacement surgery is the impact on your well-being. If hip pain makes it difficult to work, exercise, socialize, travel, or even enjoy simple daily activities, you deserve a solution that restores comfort and mobility. Many patients report feeling like they “got their life back” after replacement, a testament to how transformative the procedure can be.
If you are facing some of these symptoms persistently, you may benefit from hip arthroscopy and labral repair rather than continued conservative care.
How to Prepare for Your Hip Arthroscopy (Mental & Physical)
Preparing for hip arthroscopy is just as important as the procedure itself. Thoughtful mental and physical preparation can significantly influence pain levels, mobility, and overall recovery time after surgery. Patients who take an active role before surgery often experience smoother rehabilitation and more predictable outcomes. Understanding what to expect, and how to prepare, helps reduce stress and sets the foundation for long-term hip health.
-
Pre-Surgery Physical Optimization
Prehabilitation focuses on strengthening the muscles surrounding the hip joint before surgery. Improving strength and flexibility ahead of time helps support the joint immediately after surgery and can shorten arthroscopic hip surgery recovery time.
-
Selecting the Right Surgeon
Choosing a surgeon who frequently performs hip arthroscopy is a critical step in preparation. High-volume hip specialists are more familiar with complex anatomy and surgical techniques, which contributes to safer procedures and more consistent outcomes.
-
Effective Pain Management Post-Op
Understanding your post-operative pain plan before surgery helps reduce anxiety and improve early mobility. When pain is well controlled from the start, patients are more likely to move comfortably and begin rehabilitation on schedule.
-
Adherence to Physical Therapy
Physical therapy is a core part of preparation, not just recovery. Knowing the importance of post-operative PT helps patients mentally commit to the process, recognizing that therapy plays a major role in restoring strength, motion, and stability.
-
Post-Op Recovery Patience
Hip arthroscopy recovery happens gradually, and preparing mentally for a step-by-step process is essential. Patients who respect recovery timelines reduce the risk of setbacks caused by overactivity or premature return to sports or work.
-
Nutrition for Healing
Proper nutrition before surgery supports tissue repair and immune function. Diets rich in protein, vitamins, and anti-inflammatory foods help the body prepare for healing and reduce post-surgical fatigue.
-
Preparing Your Home Environment
Setting up your home before surgery improves safety and comfort during early recovery. Removing trip hazards, arranging sleeping areas, and preparing daily essentials in advance can reduce stress after surgery.
-
Asking the Right Questions
Preparing a list of questions for your surgical team helps clarify expectations and responsibilities. Understanding timelines, restrictions, and rehabilitation goals prevents confusion and improves confidence going into surgery.
-
Understanding Post-Op Restrictions
Knowing movement and weight-bearing restrictions ahead of time helps patients mentally prepare for lifestyle adjustments. Following these guidelines is essential to protect the surgical repair and support long-term success.
-
Long-Term Hip Health
Preparation includes thinking beyond the immediate recovery period. Learning about long-term strengthening, flexibility, and maintenance exercises helps protect surgical results and supports lasting hip function.
Why Hip Arthroscopy is Preferred for Athletes?
Athletes favor hip arthroscopy surgery because it:
- Preserves native anatomy
- Allows precise correction
- Supports faster return to sport
- Reduces long-term degeneration
- Supports lifetime of joint preservation in case of injury (preventing any risk of future surgeries)
This makes it superior to open surgery or early replacement for active individuals.
Did you know? Hip arthroscopy is especially effective for sports injuries because it allows precise repair of damaged structures while preserving healthy tissue, helping athletes return to activity faster with less disruption to joint mechanics.
What Happens During Hip Arthroscopy?
Hip arthroscopy is a minimally invasive, patient-friendly surgical procedure designed to diagnose and treat problems inside the hip joint while preserving healthy tissue. It is typically performed as an outpatient procedure, meaning most patients go home the same day. The surgery is done under general or regional anesthesia and usually lasts 90 minutes to a few hours, depending on the condition being treated.
Here’s a step-by-step look at what patients can expect during hip arthroscopy:
1. Anesthesia and Positioning
Before the procedure begins, anesthesia is administered to ensure comfort throughout surgery. Once asleep or fully relaxed, the patient’s leg is gently placed in a specialized traction device. This carefully creates a small amount of space (about 1 centimeter) within the hip joint, allowing the surgeon to work safely without damaging surrounding cartilage.
2. Small Incisions and Camera Placement
The surgeon then makes a few tiny “buttonhole” incisions, each usually about ¼ inch long, around the hip. Through one of these incisions, an arthroscope (a thin camera with a light source) is inserted into the joint. The camera sends real-time, magnified images to a monitor, giving the surgeon a clear view of the inside of the hip.
3. Treating the Problem
Using the camera for guidance, the surgeon inserts miniature surgical instruments through the remaining small incisions to treat the underlying issue. Depending on the diagnosis, this may include:
- Repairing or trimming a torn labrum, which helps restore hip stability
- Reshaping bone spurs (osteoplasty) to correct femoroacetabular impingement (FAI)
- Smoothing or repairing damaged cartilage
- Removing loose bone or cartilage fragments
- Clearing inflamed synovial tissue causing pain and stiffness
Each step is performed with precision to preserve the natural joint and improve long-term function.
4. Closing the Incisions
Once the necessary repairs are complete, the instruments are removed. The small incisions are closed with sutures or surgical tape and covered with a dressing. Because the incisions are minimal, scarring is usually very small and recovery tends to be faster compared to open surgery.
What Does Hip Arthroscopy Recovery Look Like?
| Recovery Phase | Timeframe | What to Expect | Patient Focus & Care Goals |
| Immediate Post-Op Phase | Day 0 – 2 weeks | Mild to moderate pain, swelling, and stiffness are common. Crutches are usually required to limit weight-bearing. | Pain control, wound care, icing, gentle range-of-motion exercises, and protecting the repaired tissue |
| Early Rehabilitation Phase | Weeks 2 – 6 | Gradual reduction in pain and swelling. Improved hip mobility. Transition from crutches to partial or full weight-bearing as advised. | Restore mobility, begin guided physical therapy, activate hip and core muscles |
| Strengthening Phase | Weeks 6 – 12 | Increased strength and stability. Daily activities become easier with minimal discomfort. | Progressive strengthening, balance training, improved gait mechanics |
| Advanced Rehabilitation Phase | 3 – 4 months | Near-normal movement with improved endurance and flexibility. Minimal to no pain during routine activities. | Sport- or activity-specific training, higher-level strengthening |
| Return to Full Activity | 4 – 6 months (sometimes longer) | Most patients return to work, sports, and exercise without restrictions, depending on procedure type. | Full functional recovery, injury prevention, long-term joint protection |
Risks and Potential Complications of Hip Arthroscopy
While hip arthroscopy surgery is considered safe and minimally invasive, no surgical procedure is entirely without risk. Understanding potential complications helps patients make informed decisions and recognize warning signs early.
Possible hip arthroscopy complications include infection, bleeding, blood clots, nerve irritation, stiffness, persistent pain, or incomplete symptom relief. Temporary numbness around the thigh or groin can occur due to traction used during surgery but usually resolves over time.
At high-volume centers like Detroit Ortho Doc, careful surgical planning, precise technique, and structured rehabilitation significantly reduce complication rates. Patient selection and adherence to post-operative guidelines also play a critical role in minimizing risk.
Benefits of Hip Arthroscopy – Why do we prefer Hip Arthroscopy at DetroitOrthoDoc?
The primary goal of hip arthroscopy is to restore function while preserving the natural joint. Compared to open surgery or early joint replacement, arthroscopy offers several advantages hence why it is the preferred method of hip pain management:
- Minimally Invasive Approach:
Performed through small incisions, hip arthroscopy minimizes soft tissue disruption and reduces surgical trauma compared to open procedures. - Less Postoperative Pain:
Smaller incisions and precise techniques typically result in lower pain levels and decreased need for prolonged pain medication. Since this method is often preferred for young adults, the pain is less, and recovery is much smoother too. - Faster Recovery Time:
Most patients return home the same day and progress through rehabilitation more quickly than with traditional hip surgery. - Minimal Scarring:
“Buttonhole” incisions heal with little visible scarring, offering both functional and cosmetic benefits. - Accurate Diagnosis and Treatment:
A high-definition camera allows surgeons to clearly visualize the joint and precisely address labral tears, bone impingement, and cartilage damage. - Joint Preservation:
The procedure focuses on repairing and preserving the natural hip joint rather than replacing it, making it ideal for younger and active individuals. - Improved Hip Function and Stability:
Correcting structural issues helps restore normal movement, reduce mechanical symptoms, and enhance joint stability. - Lower Risk of Complications:
Compared to open surgery, hip arthroscopy carries a reduced risk of infection, blood loss, and muscle damage. - Potential to Delay Arthritis Progression:
By addressing underlying mechanical problems early, hip arthroscopy may help slow degenerative changes within the joint. - Return to Active Lifestyle:
Many patients are able to resume work, daily activities, and sports with improved comfort, strength, and confidence.
Conclusion: Hip Arthroscopy – The Faster Route to Mobility
Hip arthroscopy is a minimally invasive, joint-preserving procedure that offers effective treatment for labral tears, femoroacetabular impingement, cartilage damage, and other structural hip conditions. By combining advanced surgical techniques, precision diagnostics, and personalized rehabilitation, patients can experience reduced pain, improved hip function, and a faster return to daily activities and sports.
At DetroitOrthoDoc, our approach emphasizes non-surgical care first and recommends arthroscopy only when conservative treatments are insufficient, ensuring the best long-term outcomes for your hip health. Whether you are an athlete or an active adult, hip arthroscopy provides a safe, effective path to restoring mobility and quality of life.